
Craniocervical/Atlanto-axial Instability
Craniocervical Instability (CCI), also known as the Syndrome of Occipitoatlantialaxial Hypermobility. Due to the instability in the craniocervical junction deformation can occur to the brainstem, upper spinal cord, and cerebellum. Primarily this occurs in patients with Ehlers-Danlos (EDS) with claims of up to 1 in 15 people with EDS likely to develop CCI [1]. It can be exacerbated in EDS patients who have a Chiari decompression due to the removal of bones in the craniocervical junction combined with the poor collagen. With the 2021 consensus paper, it become recognised that those with Chiari 1.5/Complex Chiari are at risk of also having instability that needs to be checked for. It also agrees that for those patients with both that a fusion may be required as a treatment. This is a major change and a welcome one as many Chiari patients with instability have run into a lot of trouble. Even when getting treatment for the instability years later the Chiari decompression impacts the areas mainly used for fusing. So it is better to plan out both at the same time for the best outcome.
Atlanto-axial Instability (AAI) occurs when there is excessive movement at the junction between C1 (atlas) and C2 (axis). This can occur by itself or in conjunction with CCI. Treatment includes conservative treatment or C1-C2 fusion.
Cranial Settling (CS) occurs when the ligaments in the neck are too weak and the skull slides down. Basilar invagination is usually seen in CS. Treatment includes conservative management or C0-spine fusion. This can occur with both CCI.
Retroflexed Odontoid (RO) loose ligaments impact the angle of the odontoid bone resulting in it pushing backwards and into the brainstem. A common finding in CCI.
Basilar Invagination (BI) occurs when the tip of the odontoid process migrates up past the McRae line into the skull This can cause narrowing of the foramen magnum and pressure on the brainstem.
Symptoms:
- Bobble Head/Heavy Headache
- Chiari type headache worsened by Valsalva manoeuvres
- Neck Pain (usually severe)
- Central or Mixed Sleep Apnoea
- Facial Numbness and/or pain
- Coordination/Balance Issues
- Muscle Weakness
- Dizziness and/or vertigo
- Double Vision
- Reduced Gag Reflex
- Tinnitus and/or hearing loss
- Nausea and/or vomiting
- Paralysis
- Death (rare)

CCI/AAI Awareness Ribbon
Diagnosis
Medical imaging required for the diagnosis of CCI/AAI is done via an MRI of the craniocervical junction and CT imaging with the neck in neutral, flexion, extension and rotational positions. Upright MRI's can also be used to identify the effects of gravity and having MR images with the neck in different positions like the CT. While other imaging such as the Digital Motion X-ray (DMX) is mentioned frequently in online groups this only seems to be used by certain chiropractors. There have been questionable diagnoses occurring despite both the MRI and CT being cleared by the top doctors treating CCI. Australian surgeons and the main international surgeons do NOT use DMX. So due to DMX being irrelevant for Chiari, Syringomyelia and questionable in CCI/AAI we do not have any information on local DMX. We recommend you ask the treating doctor what imaging they want to save yourself time and money.
The following measurements are frequently used to assess both instability and the degree of brainstem compression. As with imaging, there is no consensus on which angles are the best to use to allow for diagnosis.
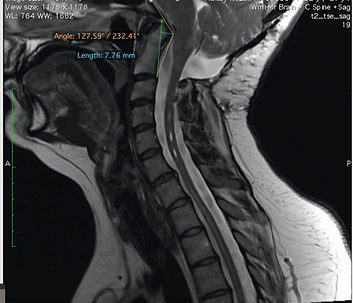
Clivo Axial Angle (CXA) - A line along the clivus and a second one down on the posterior side of the axis. (Abnormal: <150 degrees in flexion and 180 degrees in extension) This angle alone can does NOT equal a diagnosis of CCI
Basion Axial Interval (BAI) - Basion to the posterior line of axis. (Pathological: > 12 mm)
Basion-Dens Interval (BDI)- Distance between basion and tip of dens. (Pathological: > 12 mm)
Harris - BDI + BAI (Pathological: > 12 mm) *Additional, the BAI should be measured in flexion and extension. If the value varies by more than 1-2 mm this means that the head is sliding backwards and forward on the cervical spine.
Grabb-Oakes - To diagnose brainstem compression. A line on middle sagittal MRI scans from the lowest point of the clivus to the lowest posterior point of the axis corpus. Measure in a right angle from this line to the beginning of the spinal canal. (Pathological: > 8 mm)
McGregor's Line - Draw a line from the upper surface of the posterior edge of the hard palate to the posterior lowest point of the occiput. If the tip of the dens is more than 4,5 mm above the McGregors line then a basilar invagination is likely.
McRae line - Drawn on a lateral skull radiograph or mid-sagittal section of CT or MRI, joining the basion and opisthion. (Abnormal tip of dens <5mm below this line)
Powers Ratio - Distance between the basion and posterior arch of atlas divided by distance between opisthion and anterior arch of the atlas. (Pathological: > 1)
Bulls Angle - the line between the posterior and anterior arch of C1 → angle between this line and hard palate. (Pathological: > 13 degrees)
Wackenheims Line - Angle between clivus line and dural canal. This line should go through the dens or be tangential to it.
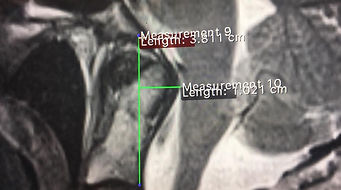
Grabb-Oakes Measurement Example
.png)
Clivio-Axial Angle Example
Mouse Roll Over: This is an example of areas used for measuring, not a tool to be used for accurate measuring
Treatment
Conservative treatment with physiotherapy, traction and/or a hard collar can be used. The most common treatment is the surgical fusion of the skull to the neck. Some patients may need the fusion extended further down their spine based on how far down the spinal instability occurs. During a CCI fusion, the skull is positioned into the optimal position and range of motion is limited afterwards. There is a range of surgical techniques used by doctors to create a fusion.




